Attention A T users. To access the menus on this page please perform the following steps.
1. Please switch auto forms mode to off.
2. Hit enter to expand a main menu option (Health, Benefits, etc).
3. To enter and activate the submenu links, hit the down arrow.
You will now be able to tab or arrow up or down through the submenu options to access/activate the submenu links.
Locator
Contact
Search
Menu
Menu
- MIRECC / CoE
- MIRECC / CoE Home
- Education
- Fellowships
- MIRECC-CoE Awards
- VISN 1 New England MIRECC
- VISN 2 Center for Integrated Healthcare
- VISN 2 CoE - Suicide Prevention
- VISN 2 New York MIRECC
- VISN 4 Philadelphia and Pittsburgh MIRECC
- VISN 5 Capitol MIRECC
- VISN 6 Mid-Atlantic MIRECC
- VISN 16 South Central MIRECC
- VISN 17 CoE - Returning War Veterans
- VISN 19 Rocky Mountain MIRECC
- VISN 20 Northwest MIRECC
- VISN 21 Sierra Pacific MIRECC
- VISN 22 Desert Pacific MIRECC
- VISN 22 CoE - Stress and Mental Health
- CESATE – Seattle
- NCPTSD
- More Health Care
- Veterans Health Administration
- Health Benefits
- Conditions & Treatments
- Wellness Programs
- Locations
- Research
- Special Groups
- Careers, Job Help & Training
- About VHA
VA Center for Integrated Healthcare (CIH)

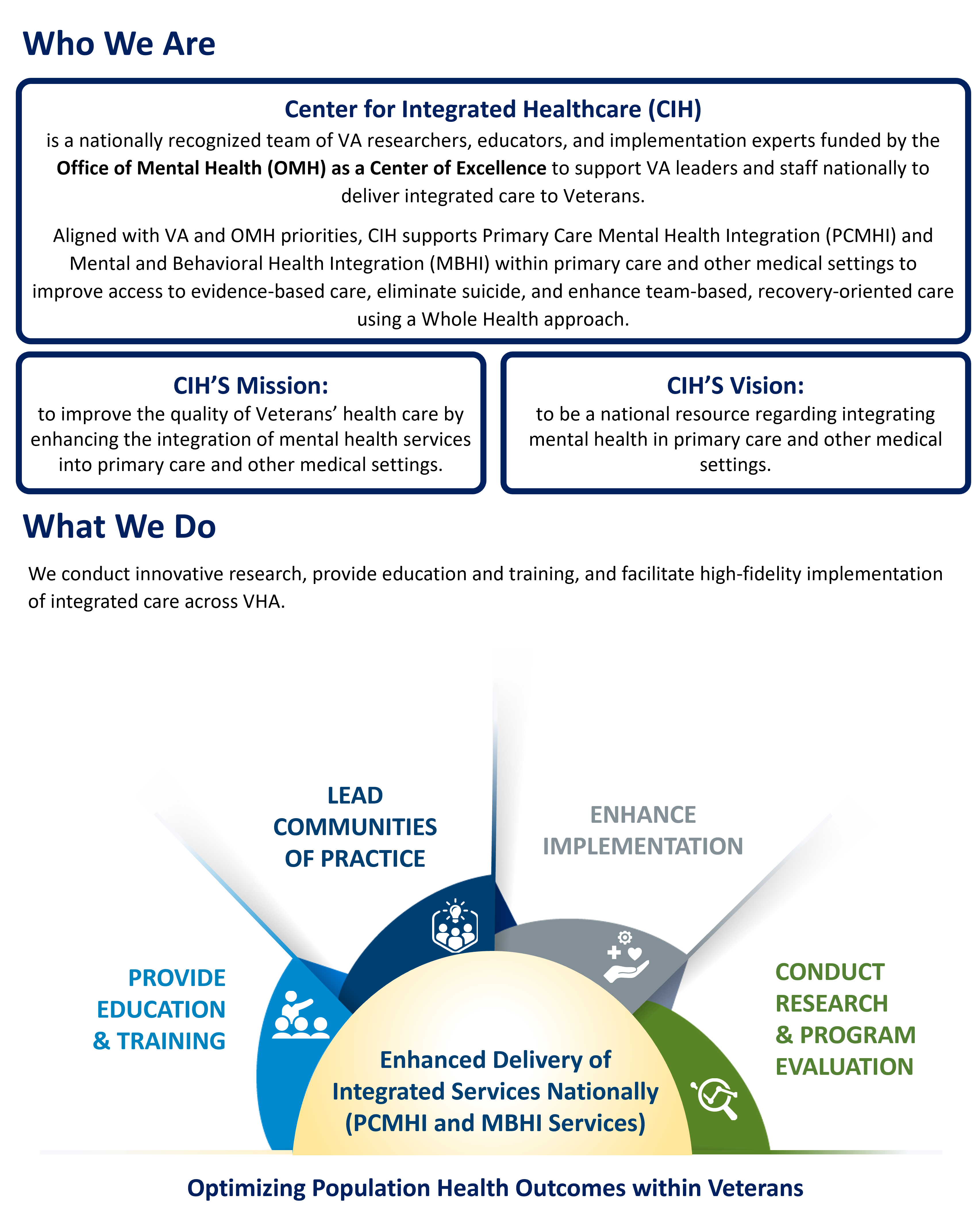
For more information: VA staff, please access our internal VA CIH SharePoint. For those external to VA, please email us at VHA CIHConsultation@va.gov.



















