MIRECC / CoE
Implementation Research | Rocky Mountain MIRECC for Suicide Prevention
 |
|||
 |
 |
 |
 |
The Rocky Mountain Mental Illness Research, Education and Clinical Center (MIRECC) for Suicide Prevention carries out research in both the Rocky Mountain Regional VA and Salt Lake City VA. We also partner across the U.S. with other VA sites, the Department of Defense and in local communities. Our research has informed changes to policy and practice throughout VHA and the community. Keep reading to learn more and see specific examples of our research.
Our Research Focus Areas
Suicide is complicated and has multiple causes. We study suicide from multiple angles, looking at factors that might put a Veteran at risk for suicide, as well as factors that help protect Veterans from suicidal thoughts or behaviors.
Our research covers a wide range of topics related to suicide prevention, including the neurobiology of suicide, clinical and behavioral interventions targeting suicidal behavior, tailoring treatments to diverse Veteran populations and implementation of evidence-based practices for suicide prevention. Our programs and research are also aligned with the National Strategy for Preventing Veteran Suicide.
Implementation of Evidence-Based Practices

Once we know that an intervention or practice is effective, we test how best to implement the practice within a certain population or setting. Implementation also includes suicide prevention strategies being carried out within communities. Below are a few specific implementation studies that the Rocky Mountain MIRECC helps to facilitate and evaluate.
In addition to implementation research, we also offer recommendations for successful adoption of suicide prevention best practices, hosted on our Clinical Practice Guidelines website. The focus of this website is to help translate the VA/DoD Clinical Practice Guideline (CPG) for Patients at Risk of Suicide into applicable strategies for Veteran care (including tools and tips for screening, evaluation, treatment and case management). The CPG website also features downloadable resources, such as the CPG Pocket Guide, and details for accessing past and upcoming sessions of the CPG Webinar Series.
Standardized Suicide Risk Screening and Evaluation (VA Risk ID)
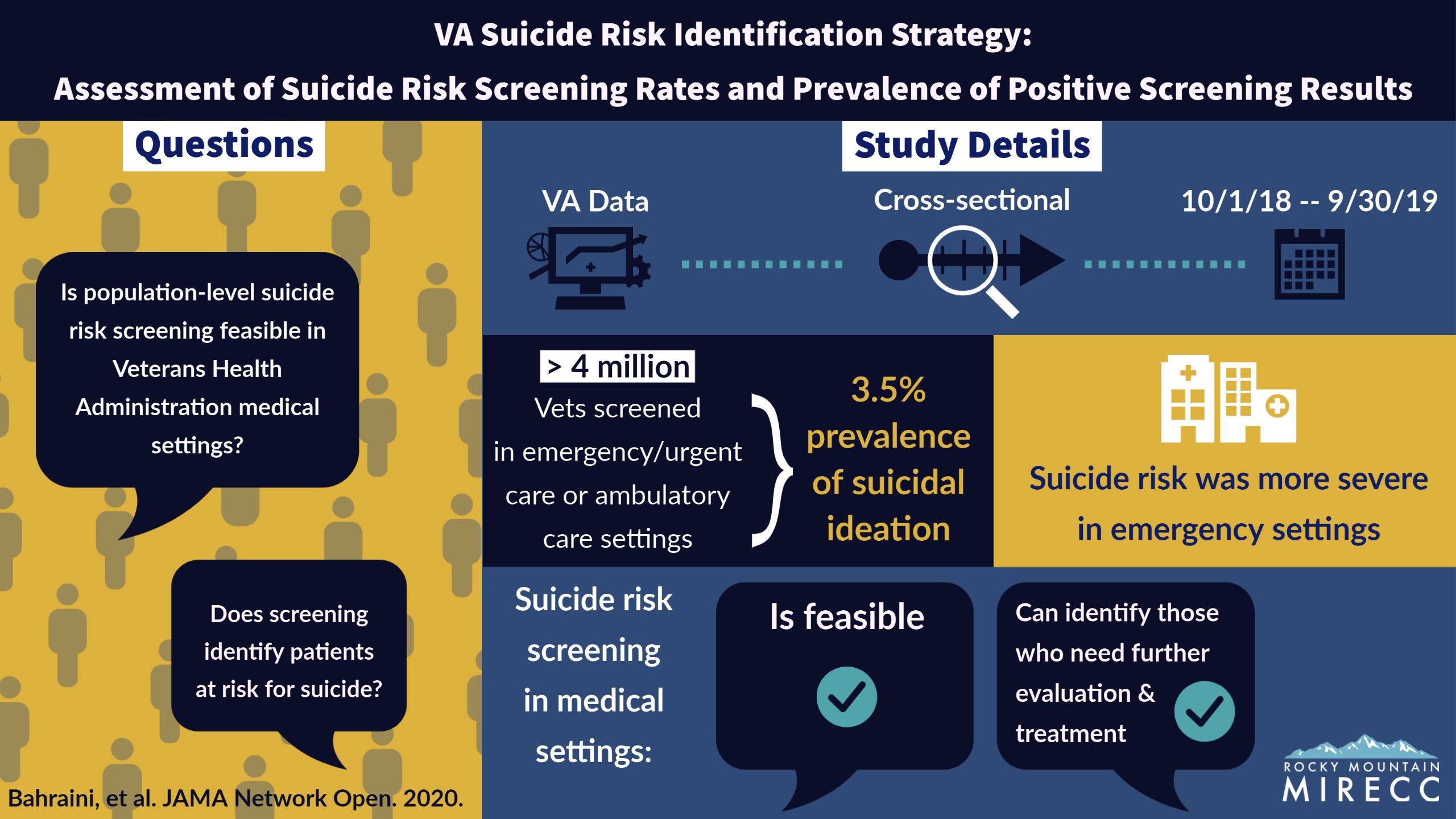
The VA Suicide Risk Identification Strategy (Risk ID) is a VHA-wide effort to develop and implement a national, standardized process for suicide risk screening and evaluation, using high-quality, evidence-based tools and practices. Rocky Mountain MIRECC provides critical implementation support for this program through weekly technical assistance calls covering pertinent suicide screening and evaluation topics and common implementation questions and challenges. An online resource library includes the most recent Risk ID guidance, best practices, training and answers to frequently asked questions. The Rocky Mountain MIRECC team is also examining the effectiveness of different strategies to increase implementation of Risk ID across healthcare settings through a QUERI Partnered Evaluation Initiative. This program and its associated studies are in the clinical implementation phase.
This visual outlines findings from an early study of the Risk ID program. Click the image to enlarge and learn more.
Using a Predictive Model for Suicide Risk Identification and Intervention (REACH VET)
REACH VET (Recovery Engagement and Coordination for Health – Veterans Enhanced Treatment) utilizes a predictive model to identify Veterans who may benefit from enhanced clinical care, outreach and risk assessment. REACH VET and its associated studies are in the clinical implementation phase. Rocky Mountain MIRECC supports the implementation of REACH VET through educational calls that cover topics pertinent to REACH VET coordinators, such as monthly metrics updates and examples of best practices. Coordinators can also contact the REACH VET implementation team for specific questions and assistance and have access to an online library of resources that includes guidance documents, training, sample letters and more.
Supporting Patients after Discharge from the Emergency Department (SPED)
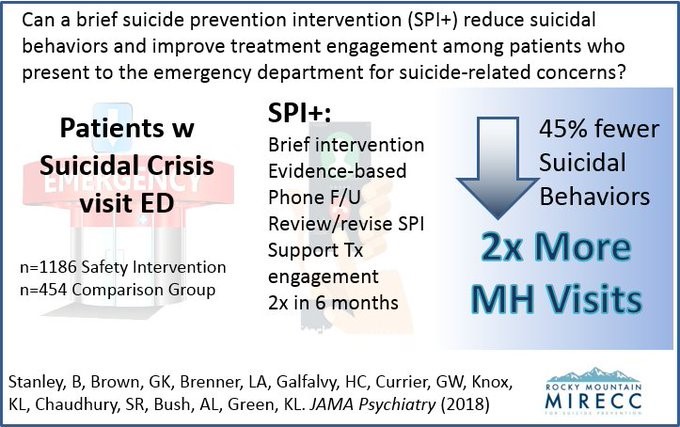
Patients who are treated in an Emergency Department (ED) are at increased risk of subsequent suicide, even if the reason for visit is not due to suicidal thoughts or behavior. Safety Planning in the ED (SPED) is based on an intervention developed and studied by Stanley (Columbia University) and Brown (University of Pennsylvania), in collaboration with Rocky Mountain MIRECC’s Director, Dr. Lisa Brenner. The intervention was associated with a 45% reduction in suicidal behavior in the 6 months following ED discharge. As part of the intervention, patients complete a safety plan while in the ED and receive weekly provider contact (including risk assessment, safety planning, identification of barriers to care) until the patient is engaged in mental health care.
Rocky Mountain MIRECC supports the implementation of SPED through educational calls that cover SPED guidance and frequently asked questions and allow time for providers to talk through specific clinical scenarios and implementation barriers and facilitators. Providers in the field also have access to an online resource library that includes best practices, video role plays, staff-specific guidance and more.
This podcast and visual abstract provide more info on SPED.
- Click image to enlarge and learn more about SPED.
- Podcast: Safety Planning in the Emergency Room (it works!)
Community-Based Suicide Prevention
There are many Veterans who receive some or all of their care from outside of the Veterans Health Administration (VHA). Because of this, investigators at the Rocky Mountain MIRECC have created community-based programs to help understand the treatment needs of these Veterans and the ways we can support organizations providing outside care. By collaborating with organizations in the community, we aim to increase continuity and accessibility of critical suicide prevention care so that Veterans may receive it where they are most comfortable.
Together with Veterans
How can Veterans help other Veterans manage mental, emotional and practical aspects of mental health and suicide prevention? Together with Veterans is a community-based suicide prevention program for rural Veterans. It is Veteran-driven, collaborative, evidence-informed and community-centered. This program is in the public health phase of the translational science spectrum. This visual shows how Together with Veterans works in communities to support rural Veterans.
Click the image to enlarge and learn more.
Patient Safety Center of Inquiry-VA Suicide Prevention Collaborative (PSCI-VASPC)
Veteran’s Health Administration (VHA) has built a robust system of Veteran suicide prevention outreach and intervention programming. Yet major gaps exist for Veterans who are not eligible for, or do not choose to enroll in VHA care. In response Dr. Bryann DeBeer and colleagues developed the Patient Safety Center of Inquiry – Suicide Prevention Collaborative (PSCI-SPC). This VHA-community collaborative partnership works to develop, implement and evaluate practical solutions to the rising rate of suicide among non-VHA using Veterans. Learn more from the following publication, podcast, and article featuring PSCI-SPC.
- Suicide Prevention Collaboration: Creating novel approaches to suicide prevention among Veterans receiving community services
- Podcast: Community Partnerships for Preventing Veteran Suicide
- VHA Community Partnership Challenge - National Center for Healthcare Advancement and Partnerships (PSCI-SPC one of three winning programs)
Our clinical implementation research includes the Clinical Implementation and Public Health phases of the translational model. Visit the translational model page to learn more about these and other phases in the model.

Explore other research focus areas
Research Findings
The documents listing publications from Rocky Mountain MIRECC-affiliated research are currently down for extended maintenance while we improve the accessibility. Thanks for your patience and we apologize for the inconvenience.
Questions? We strive to make our content accessible to all, and we know you may be temporarily unable to find the publications that used to be available here. If we can assist you while the page is down and for any questions about the publications web maintenance, please contact us at RockyMountainMIRECC@va.gov.
Quick Links to Study Websites
- Understanding Transgender and Gender Diverse Veterans’ Experiences, Needs, and Preferences
- VA Patient Safety Center of Inquiry - Suicide Prevention Collaborative (PSCI-SPC)
- Home-Based Measurement of Circadian Timing in Veterans with Traumatic Brain Injury and Insomnia (Home Circadian)
- Promoting mental health wellness and safety among Veteran firearm owners (FFAST)
- Assessing Social & Community Environments with National Data (ASCEND)
- Suicide Risk and Prevention among Asian American and Pacific Islander Veterans
- Military and Veteran Microbiome: Consortium for Research and Education (MvM CoRE)
- Facilitating Assessment of At-Risk Sailors using Technology (FAAST)
- Advancing Suicide Prevention for Underserved Veterans (ASPIRE) Lab
Site Map
Last Updated 14 December 2021