MIRECC / CoE
Clinical Intervention Research | Rocky Mountain MIRECC for Suicide Prevention
 |
|||
 |
 |
 |
 |
The Rocky Mountain Mental Illness Research, Education and Clinical Center (MIRECC) for Suicide Prevention carries out research in both the Rocky Mountain Regional VA and Salt Lake City VA. We also partner across the U.S. with other VA sites, the Department of Defense and in local communities. Our research has informed changes to policy and practice throughout VHA and the community. Keep reading to learn more and see specific examples of our research.
Our Research Focus Areas
Suicide is complicated and has multiple causes. We study suicide from multiple angles, looking at factors that might put a Veteran at risk for suicide, as well as factors that help protect Veterans from suicidal thoughts or behaviors.
Our research covers a wide range of topics related to suicide prevention, including the neurobiology of suicide, clinical and behavioral interventions targeting suicidal behavior, tailoring treatments to diverse Veteran populations and implementation of evidence-based practices for suicide prevention. Our programs and research are also aligned with the National Strategy for Preventing Veteran Suicide.
Clinical Interventions

Our investigators explore a range of treatments and clinical interventions that may treat suicidal thoughts and behaviors both directly and indirectly. Direct interventions include treatments that specifically target suicide ideation or behaviors. Indirect interventions, on the other hand, often address suicide risk factors, including co-occurring medical and mental health conditions. Treating these “indirect” causes may help reduce overall suicide risk or improve the effectiveness of direct interventions.
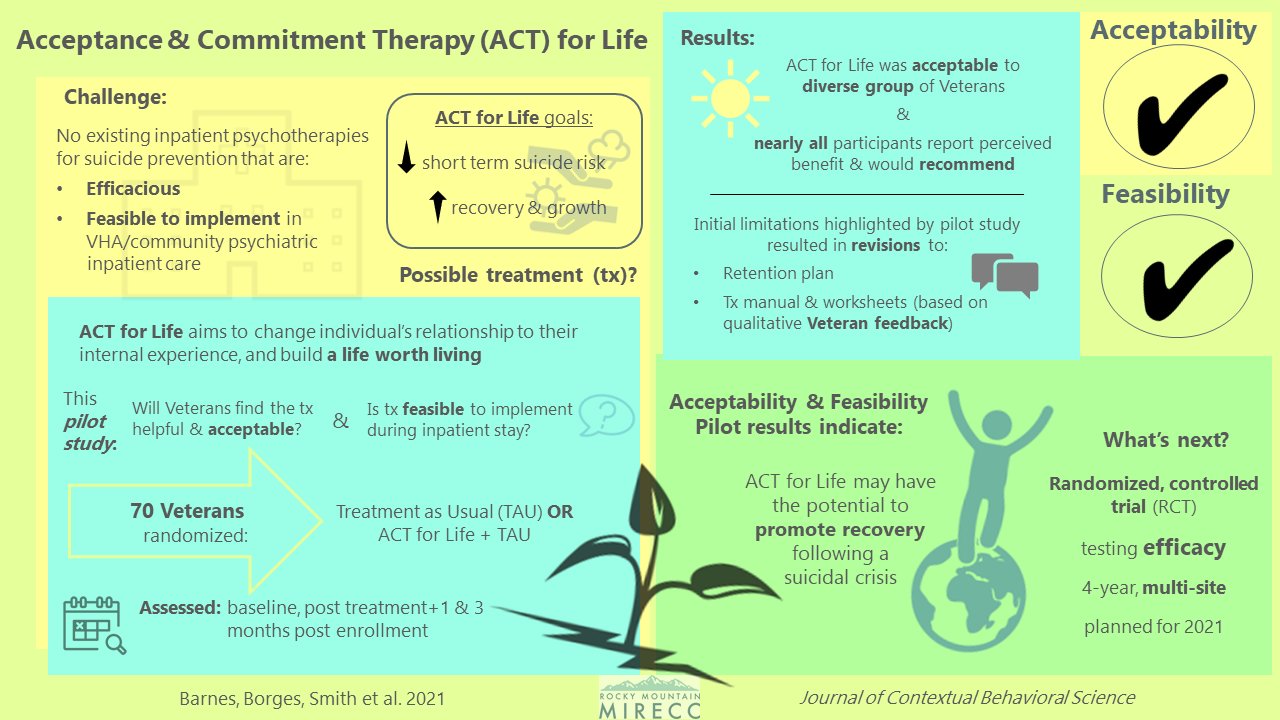
Acceptance & Commitment Therapy (ACT) for Life
Dr. Sean Barnes and his team are studying a treatment called Acceptance & Commitment Therapy (ACT) for Life, with the goal of reducing suicide risk and helping Veterans build a life worth living. This treatment can be especially powerful during a Veteran’s transition from inpatient hospital care back to home or outpatient care. ACT studies are in the clinical research phases, which means these interventions are being tested to see if they are effective in reducing suicide risk and increasing functioning for Veterans.
- Click the image to enlarge and learn more about the conclusions from the pilot study.
- Podcast: Beyond Prevention — Acceptance and Commitment Therapy for Life
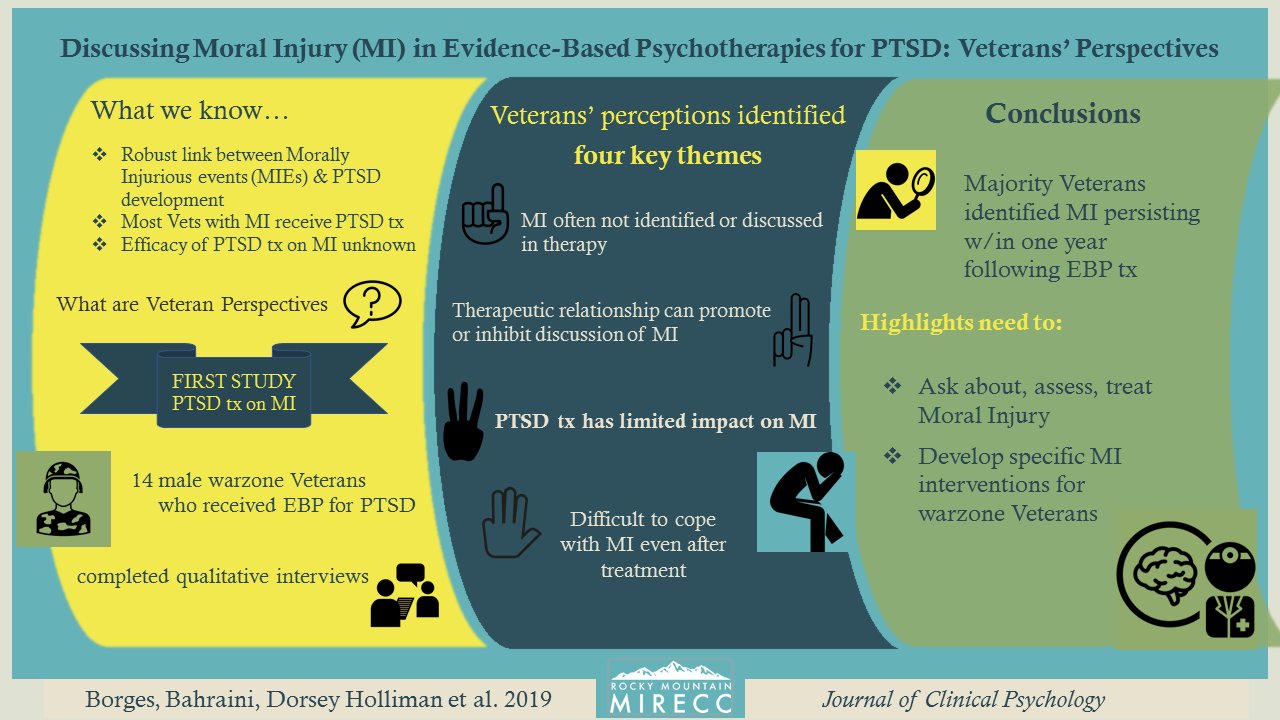
Acceptance & Commitment Therapy (ACT) for Moral Injury
Many Veterans who report experiences of moral injury have received treatment for PTSD. But there is not a treatment that specifically addresses moral emotions like guilt, shame, disgust and anger. Dr. Borges and her team are studying if ACT for Moral Injury helps Veterans recover after their morals are violated in the warzone. Like ACT for Life, this study is also part of the clinical research phase. The visual abstract below shows Veterans’ perspectives leading to development of a moral injury specific treatment.
Click the image to enlarge and learn more.
Insomnia and Suicide Prevention: New Approaches for Treatment
Insomnia has been shown to directly and indirectly impact suicide risk. This means that effectively treating insomnia can help reduce overall suicide risk and symptoms of other mental health conditions (e.g., depression, PTSD, anxiety). Cognitive Behavioral Therapy for Insomnia (CBT-I) is one of the most efficacious treatments for insomnia; however, access to CBT-I is severely limited by a lack of trained clinicians. Several Rocky Mountain MIRECC investigators have conducted research to expand access to CBT-I by delivering the treatment in new ways. Learn more about promising new approaches to insomnia treatment in the context of suicide prevention from the following resources.
Our clinical intervention research is primarily within the Clinical Research phase of the translational model. Visit the translational model page to learn more about this and other phases in the model.

Explore other research focus areas
Research Findings
The documents listing publications from Rocky Mountain MIRECC-affiliated research are currently down for extended maintenance while we improve the accessibility. Thanks for your patience and we apologize for the inconvenience.
Questions? We strive to make our content accessible to all, and we know you may be temporarily unable to find the publications that used to be available here. If we can assist you while the page is down and for any questions about the publications web maintenance, please contact us at RockyMountainMIRECC@va.gov.
Quick Links to Study Websites
- Understanding Transgender and Gender Diverse Veterans’ Experiences, Needs, and Preferences
- VA Patient Safety Center of Inquiry - Suicide Prevention Collaborative (PSCI-SPC)
- Home-Based Measurement of Circadian Timing in Veterans with Traumatic Brain Injury and Insomnia (Home Circadian)
- Promoting mental health wellness and safety among Veteran firearm owners (FFAST)
- Assessing Social & Community Environments with National Data (ASCEND)
- Suicide Risk and Prevention among Asian American and Pacific Islander Veterans
- Military and Veteran Microbiome: Consortium for Research and Education (MvM CoRE)
- Facilitating Assessment of At-Risk Sailors using Technology (FAAST)
- Advancing Suicide Prevention for Underserved Veterans (ASPIRE) Lab
Site Map
Last Updated 14 December 2021