MIRECC / CoE
Our Research | Rocky Mountain MIRECC for Suicide Prevention
 |
|||
 |
 |
 |
 |
The Rocky Mountain Mental Illness Research, Education and Clinical Center (MIRECC) for Suicide Prevention carries out research in both the Rocky Mountain Regional VA and Salt Lake City VA. We also partner across the U.S. with other VA sites, the Department of Defense and in local communities. Our research has informed changes to policy and practice throughout VHA and the community. Keep reading to learn more and see specific examples of our research.
Our Research Focus Areas
Suicide is complicated and has multiple causes. We study suicide from multiple angles, looking at factors that might put a Veteran at risk for suicide, as well as factors that help protect Veterans from suicidal thoughts or behaviors.
Our research covers a wide range of topics related to suicide prevention, including the neurobiology of suicide, clinical and behavioral interventions targeting suicidal behavior, tailoring treatments to diverse Veteran populations and implementation of evidence-based practices for suicide prevention. Our programs and research are also aligned with the National Strategy for Preventing Veteran Suicide.
Neurobiology of Suicide

Our research into the neurobiology of suicide uses approaches such as brain imaging, animal models and data from public health records to examine how the brain’s structure and biochemistry may impact suicidal thoughts and behavior.
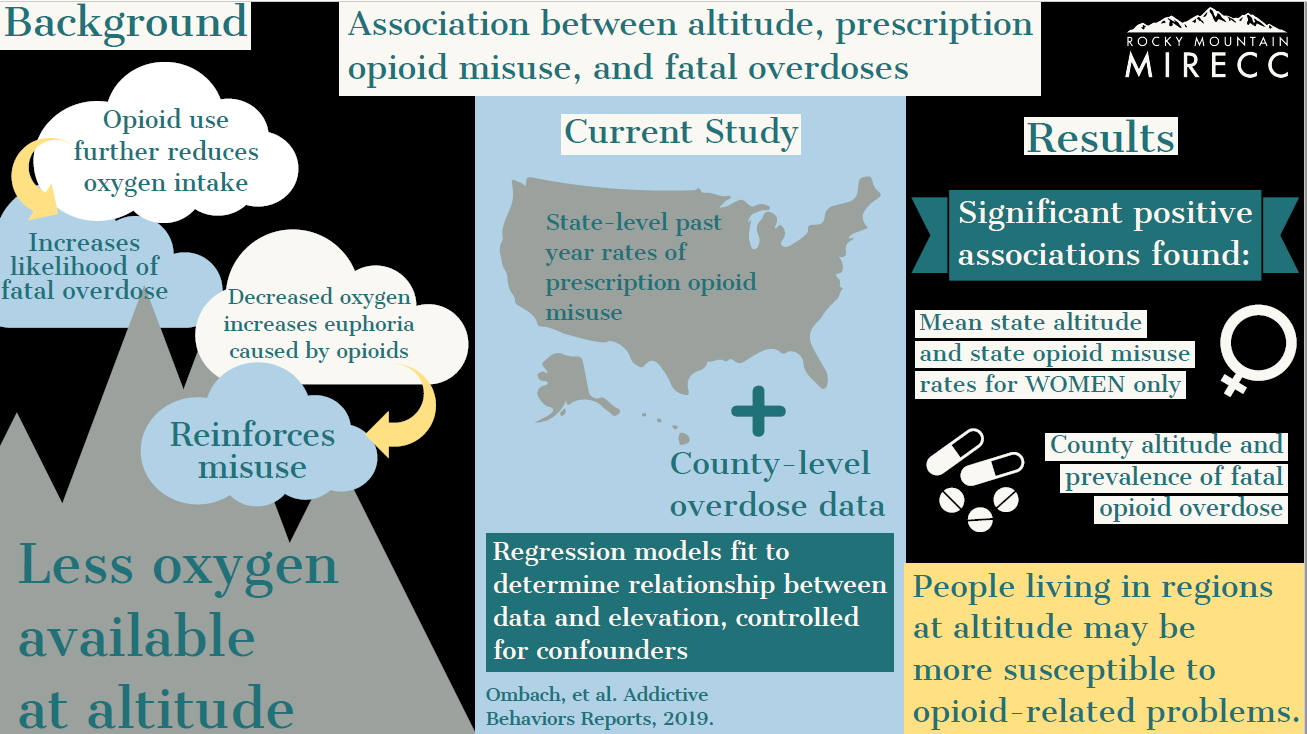
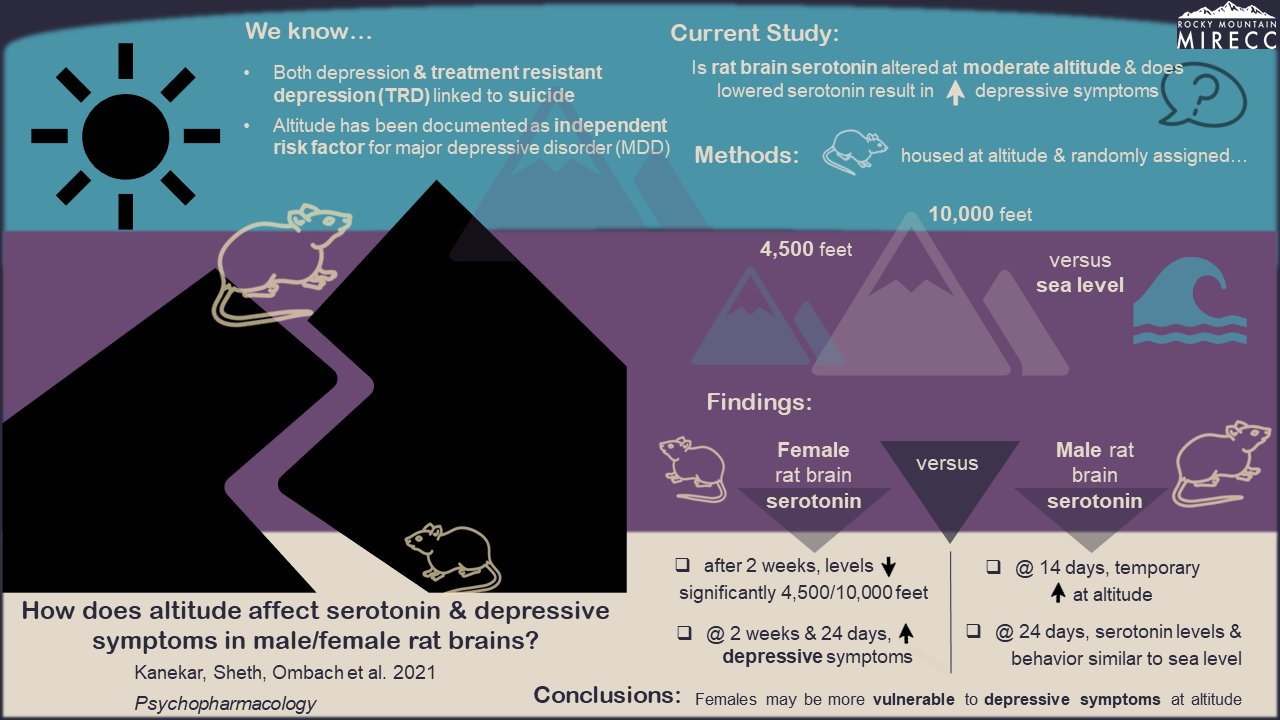
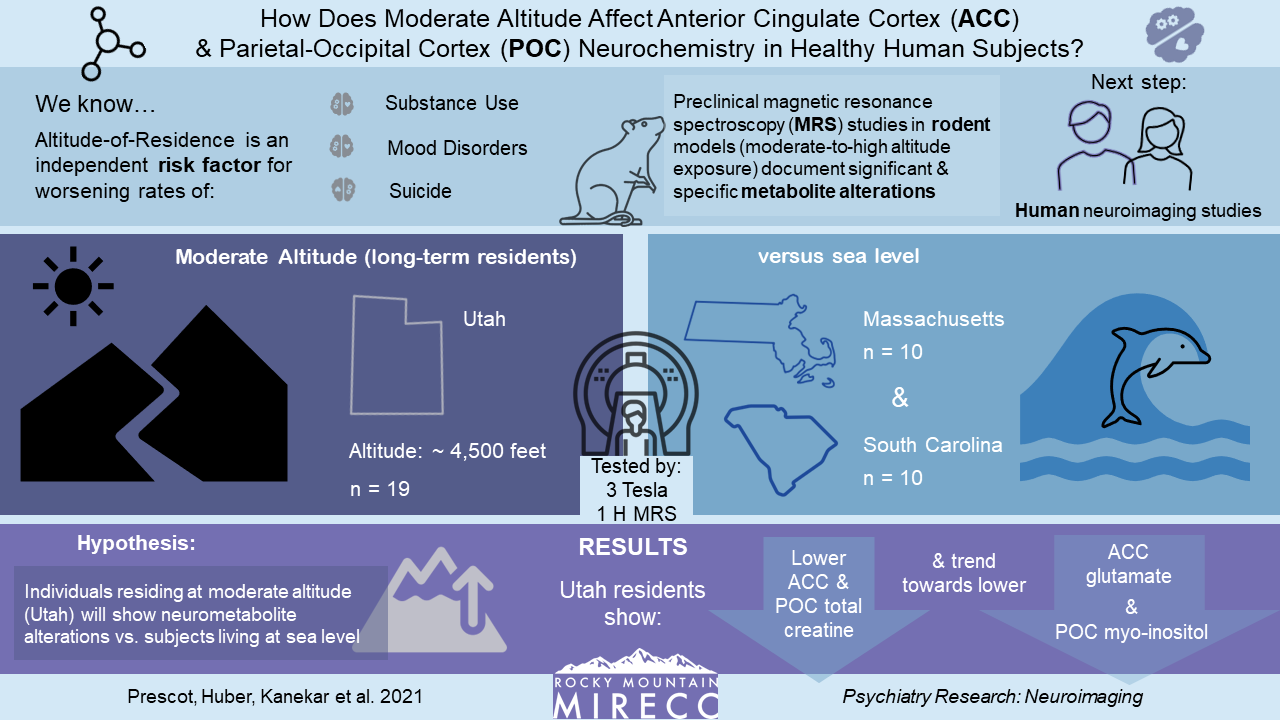
Hypoxia & Altitude
Several of our studies have explored how chronic hypoxia (lack of oxygen) resulting from living at high altitude may affect psychiatric disorders and treatments related to suicide. The graphics below give more information about studies conducted by researchers at our Salt Lake City site.
Click the images to enlarge and learn more.
Creatine Supplementation
Creatine supplementation has the potential to improve disruptions in brain energy that are implicated in the development and maintenance of depression. This visual abstract highlights one study in this area, conducted by Drs. Douglas Kondo and Perry Renshaw.
Click the image to enlarge and learn more.
Our research about the neurobiology of suicide is in the Basic and Preclinical Research phases. Visit the translational model page to learn more about these and other phases in the model.

Explore other research focus areas
Quick Links to Study Websites
- Understanding Transgender and Gender Diverse Veterans’ Experiences, Needs, and Preferences
- VA Patient Safety Center of Inquiry - Suicide Prevention Collaborative (PSCI-SPC)
- Home-Based Measurement of Circadian Timing in Veterans with Traumatic Brain Injury and Insomnia (Home Circadian)
- Promoting mental health wellness and safety among Veteran firearm owners (FFAST)
- Assessing Social & Community Environments with National Data (ASCEND)
- Suicide Risk and Prevention among Asian American and Pacific Islander Veterans
- Military and Veteran Microbiome: Consortium for Research and Education (MvM CoRE)
- Facilitating Assessment of At-Risk Sailors using Technology (FAAST)
- Advancing Suicide Prevention for Underserved Veterans (ASPIRE) Lab
Research Findings
The documents listing publications from Rocky Mountain MIRECC-affiliated research are currently down for extended maintenance while we improve the accessibility. Thanks for your patience and we apologize for the inconvenience.
Questions? We strive to make our content accessible to all, and we know you may be temporarily unable to find the publications that used to be available here. If we can assist you while the page is down and for any questions about the publications web maintenance, please contact us at RockyMountainMIRECC@va.gov.
Site Map
Last Updated 20 March 2024